As with cigarette smoking, e-cigarettes have major adverse effects on the cardiovascular system. And, in contrast to cancer, these changes occur quickly. Two recent papers, Association of Electronic Cigarette Exposure on Cardiovascular Health: A Systematic Review and Meta-Analysis and Electronic Nicotine Delivery Systems and Cardiovascular/Cardiometabolic Health, provide comprehensive summaries on the specific adverse biological effects of e-cigarette use on the cardiovascular system. These changes explain why the epidemiology finds increased risks of heart attacks and other cardiovascular events.
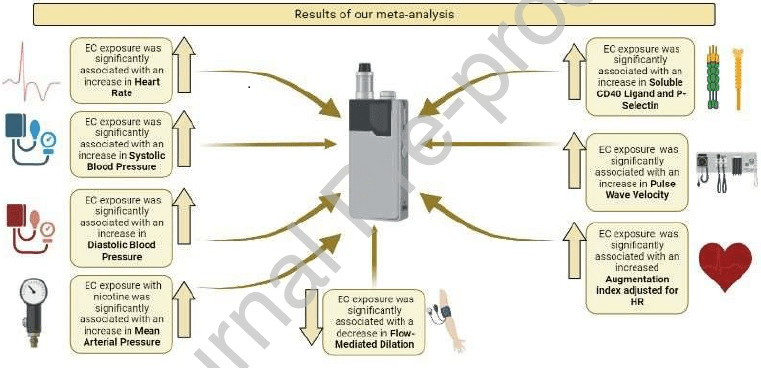
The first paper, Association of Electronic Cigarette Exposure on Cardiovascular Health: A Systematic Review and Meta-Analysis, limits itself to effects on e-cigarettes observed in people. They found that heart rate and blood pressure (systolic and diastolic) increased significantly immediately after using an e-cigarette. Over time, these changes lead to increased risk of cardiovascular disease, including coronary disease and heart failure as well as kidney disease. E-cigarette use also increases arterial stiffness (measured with pulse wave velocity and augmentation index) and lower capacity for arteries to get bigger (dilate when needed to accommodate higher blood flow, flow mediated dilation). P-selectin, which is involved in making platelets and blood vessels sticky, and CD40, which is related to inflammation, are also increased. These changes also lead to cardiovascular disease.
The second paper, Electronic Nicotine Delivery Systems and Cardiovascular/Cardiometabolic Health, describes how e-cigarettes change cellular function in ways that change the shape of the heart and the ability of heart muscle cells to contract, including formation of the proteins that comprise sarcomeres, “contractile elements” within heart cells. These changes are manifest at the whole heart level as changes in the shape of the heart and its ability to pump blood. Some of these effects differ between male and female animals, with more pronounced effects in males. The presence of other conditions, including elevated lipids or obesity, increase some of the adverse effects of e-cigarettes. Some of these changes in adipose (fat) tissue lead to changes that impact cardiac function.
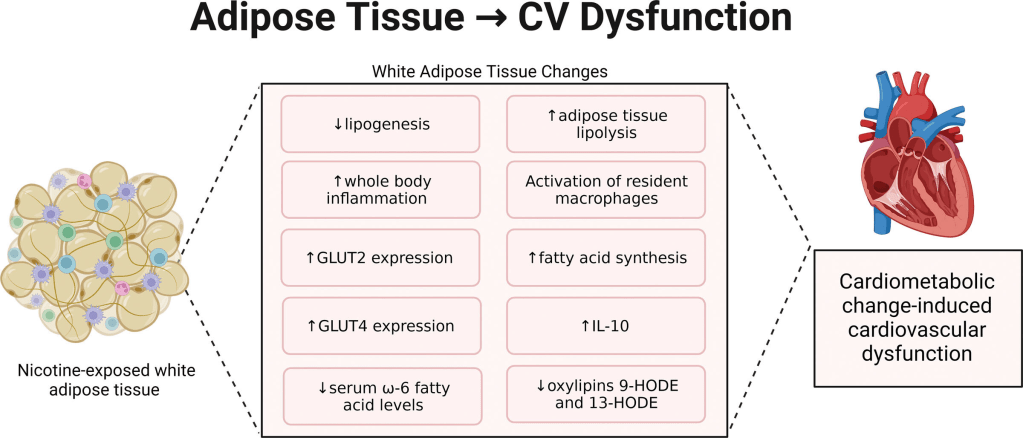
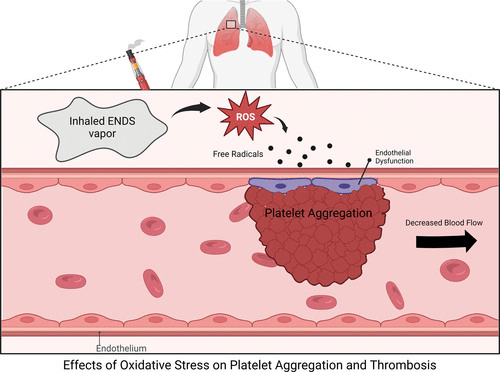
The paper also details the mechanisms through which e-cigarettes act through the central nervous system to affect heart rate and produce the changes in heart rate and platelet and vascular function that the first review documented in humans.
They also discuss the role of nicotine in causing these effects as well as differences associated with different flavors.
What these findings mean for the “causality debate”
E-cigarette advocates love to criticize epidemiology research — especially cross-sectional studies — on the grounds that they cannot prove “causation.” The fact that there is a wide range of evidence, from experimental studies in humans (where it is possible to draw causal conclusions because it is a controlled environment) all the way down to evidence at the subcellular level, on how e-cigarettes generate biological changes to lead to disease creates an important context for interpreting the epidemiology. Indeed, the increases in disease that the epidemiology studies often find are precisely what one would expect based on the biology.
Here are the full citations and abstracts:
Siddiqi TJ, Rashid AM, Siddiqi AK, Anwer A, Usman MS, Sakhi H, Bhatnagar A, Hamburg NM, Hirsch GA, Rodriguez CJ, Blaha MJ, DeFilippis AP, Benjamin EJ, Hall ME. Association of Electronic Cigarette Exposure on Cardiovascular Health: A Systematic Review and Meta-Analysis. Curr Probl Cardiol. 2023 Apr 21:101748. doi: 10.1016/j.cpcardiol.2023.101748. Epub ahead of print. PMID: 37088177. It is available here.
Despite the growing use of electronic cigarettes (EC) in the US, particularly among young people, and their perceived safety, current evidence suggests that EC usage may cause adverse clinical cardiovascular effects. Therefore, we aim to pool all studies evaluating the association of EC exposure with cardiovascular health. Medline, Cochrane CENTRAL, and Scopus were searched for studies from January 1, 2006 until December 31, 2022. Randomized and observational studies reporting cardiovascular outcomes, hemodynamic parameters and biomarkers of platelet physiology, before and after acute or chronic EC exposure were pooled using a random-effects model. Overall, 27 studies (n=863) were included. Heart rate increased significantly after acute EC exposure (weighted mean difference [WMD]: 0.76 bpm; 95% confidence interval [CI], 0.48, 1.03; p<0.00001; I2=92%). Significant increases in systolic blood pressure (WMD: 0.28 mmHg; 95% CI, 0.06, 0.51; p=0.01; I2=94%), diastolic blood pressure (WMD: 0.38 mmHg; 95% CI, 0.16, 0.60; p=0.0006; I2=90%), and PWV (WMD: 0.38; 95% CI, 0.13, 0.63; p=0.003; I2=100%) were also observed. Augmentation index increased significantly (SMD: 0.39; 95% CI, 0.11, 0.67; p=0.007; I2=90%), whereas reduction in flow-mediated dilation (WMD: -1.48; 95% CI, -2.49, -0.47; p=0.004; I2=45%) was observed. Moreover, significant rise in both soluble P-selectin (WMD: 4.73; 95% CI, 0.80, 8.66; p=0.02; I2=98%) and CD40L (WMD: 1.14; 95% CI, 0.41, 1.87; p=0.002; I2=79%) was observed. Our results demonstrate that smoking EC is associated with a significant increase in cardiovascular hemodynamic measures and biomarkers. Our findings can aid policymakers in making informed decisions regarding the regulation of EC to ensure public safety.
Mears MJ, Hookfin HL, Bandaru P, Vidal P, Stanford KI, Wold LE. Electronic Nicotine Delivery Systems and Cardiovascular/Cardiometabolic Health. Circ Res. 2023 Apr 28;132(9):1168-1180. doi: 10.1161/CIRCRESAHA.123.321565. Epub 2023 Apr 27. PMID: 37104558. It is available here.
The use of electronic nicotine delivery systems, specifically electronic cigarettes (e-cig), has risen dramatically within the last few years; the demographic purchasing these devices is now predominantly adolescents that are not trying to quit the use of traditional combustible cigarettes, but rather are new users. The composition and appearance of these devices has changed since their first entry into the market in the late 2000s, but they remain composed of a battery and aerosol delivery system that is used to deliver breakdown products of propylene glycol/vegetable glycerin, flavorings, and potentially nicotine or other additives. Manufacturers have also adjusted the type of nicotine that is used within the liquid to make the inhalation more palatable for younger users, further affecting the number of youth who use these devices. Although the full spectrum of cardiovascular and cardiometabolic consequences of e-cig use is not fully appreciated, data is beginning to show that e-cigs can cause both short- and long-term issues on cardiac function, vascular integrity and cardiometabolic issues. This review will provide an overview of the cardiovascular, cardiometabolic, and vascular implications of the use of e-cigs, and the potential short- and long-term health effects. A robust understanding of these effects is important in order to inform policy makers on the dangers of e-cigs use.
